|
At the request of listeners, we are covering some essential clinical topics such as deep neck infections including peritonsilar abscess (also known as "quinsy"). These are life-threatening conditions that require early recognition and intervention. Since peritonsilar infections are not of deep visceral spaces, this is technically separate but given their high incidence and at times coexistence with other deep neck infections they are often combined such as in discussion.
Deep neck infections are most commonly caused by a Streptococcus species, the results are often polymycrobial. It is worth noting that immunocompromised patients can have other pathogens. In additional to Streptococcus species, Klebsiella pneumonia is another common culprit and more common in elderly patients. Given the frequency of polymycrobial infections with both for aerobic and anaerobic bacteria broad spectrum antibiotics are often suggested. Clindamycin is frequently used but cephalosporins and penicillin based antibiotics with the addition of metronidazole has also been frequently recommended. However,other strategies have included the use of vancomycin when there is an increased risk for MRSA.
In a survey of 815 patients from one academic hospital, all patients had a fever on presentation (however, a fever may not always be seen in general). In descending order perimandibular edema, pain to the involved region, trismus, odynophagia, dysphagia, shivering, and respiratory distress were also present. Dental infections are a common source as well as dental procedures but tonsillitis and stones were also common causes. Another study of 330 patients found approximately 95% had abnormal findings on CBC. Positive blood cultures were found in approximately 62% of patients that had cultures obtained. Approximately 74% of patients did not receive antibiotics in that study before they came to the hospital. Traditionally, strep throat has been thought of as the usual cause that leads to peritonsilar abscesses (PTAs) but with more recent evidence, this does not seem to be the case. Whereas strep is seasonal, PTAs occur year round at a steady rate. They develop as pus accumulates between the fibrous capsule of the tonsil and the superior pharyngeal constrictor muscle. Although sometimes it may be difficult to detect with early presentation, patients with PTA and other deep neck infections areill appearing often with fever, progressively worsening throat pain, and dysphagia. Although the sore throat may be on both sides, it is worse on the affected side with pain radiating to the ipsilateral ear. Patients may also complain of difficulty swallowing and pain. The combined odynophagia and dysphagia often leads to drooling and "hot potato" voice which is classic with the disease process. Physical examination will often demonstrate trismus secondary to difficulty opening the mouth from inflammation and spasm of the masticator muscles. Marked tender cervical lymph nodes can be felt and inspection of the oropharynx reveals swelling and erythema of the anterior tonsilar pillar and soft palate on the affected side. Bilateral PTAs are rare but can occur making the diagnosis sometimes more difficult to obtain. The tonsil is generally displaced inferiorly and medially with contralateral deviation of the uvula. If not recognized or inadequately treated, life-threatening complications can occur ranging from upper airway obstruction, to abscess rupture with aspiration of pus, or with further extension of the infection into the deep tissues of the neck which will put neurologic and vascular structures at risk. Although the diagnosis is usually made clinically for PTAs and deep neck infections, confirmation by CT with IV contrast is usually beneficial when possible. PTA for example may start as cellulitis and if not recognized as such can lead to an unnecessary procedure with potential complications. CT of the soft tissues of the neck can also help in identifying potential complications. The CT soft tissue neck with IV contrast below demonstrates an approximately 3cm x 1.5cm right peritonsilar abscess with right sided cervical lymphadenopathy with the largest being 1.7cm in size.
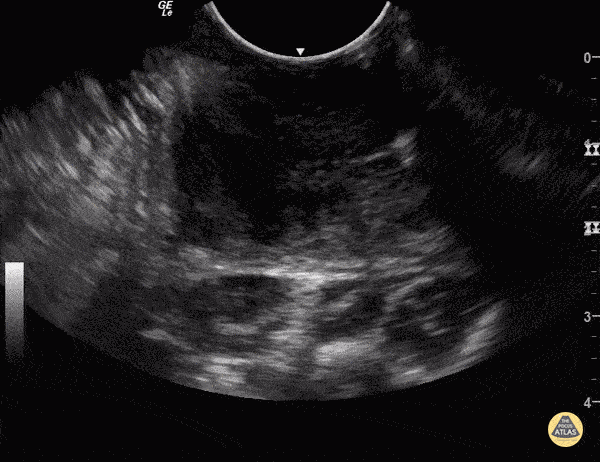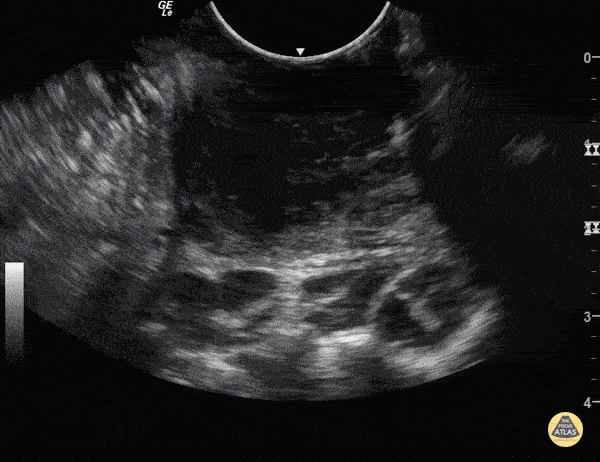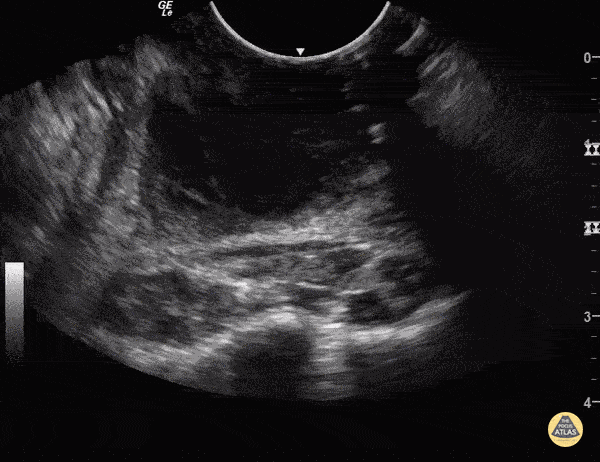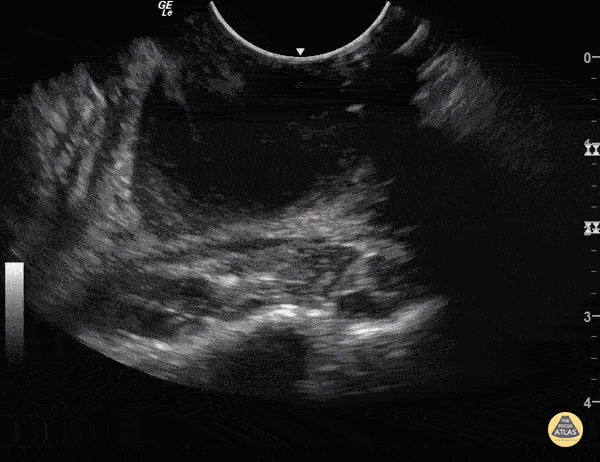
Above you will see an example of what a PTA looks like on point of care ultrasound (POCUS) with the image being available at The POCUS Atlas.
PTAs are managed with drainage of the abscess. In general with deep neck infections, surgical management along with antibiotics and supportive care are key. With PTAs, immediate tonsillectomy used to be performed but is no longer done so routinely. As a final point with PTAs, steroids are often used with some benefit. We have also covered the use of single dose dexamethasone before with Salim Rezaie on REBEL Cast and on our own podcast. Let us know what you think by giving us feedback here in the comments section or contacting us on Twitter or Facebook. Remember to look us up on Libsyn and on iTunes. If you have any questions you can also comment below, email at [email protected], or send a message from the page. We hope to talk to everyone again soon. Until then, continue to provide total care everywhere.
0 Comments
Leave a Reply. |
Libsyn and iTunesWe are now on Libsyn and iTunes for your listening pleasure! Archives
August 2022
Categories |
||||||


 RSS Feed
RSS Feed