|
Point of care ultrasound (POCUS) is becoming more widely used in a variety of musculoskeletal applications and this includes infectious pathology such as flexor tenosynovitis. In this blog and podcast, we talk about a recent paper regarding the diagnostic utility of this condition.
Before we dive into the discussion, topics such as this are covered in Practical POCUS courses including the one coming up in Missouri August 5-7, 2019. Register for Critical Access 2019 during their flash sale and save an additional 10% on the course.
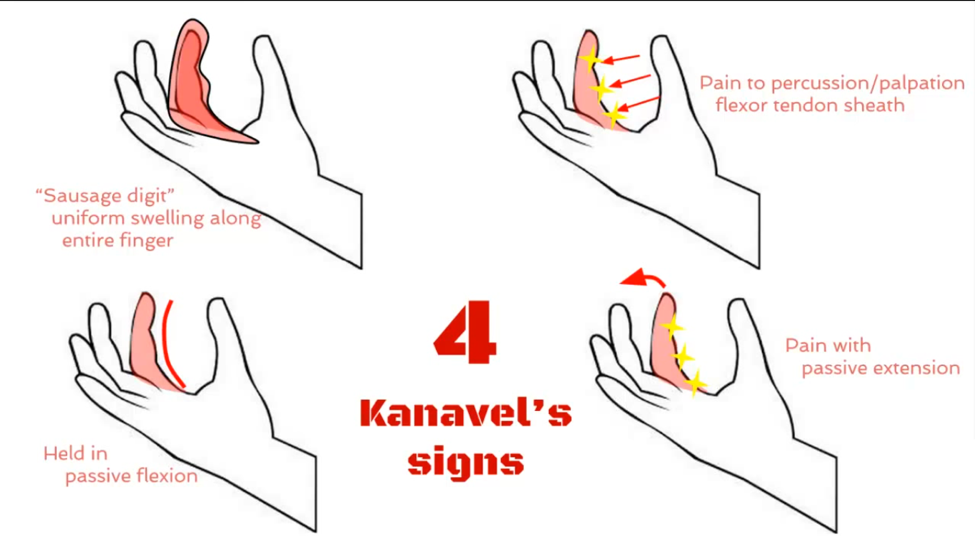
Flexor tenosynovitis is a serious infection that usually requires surgical intervention. Classically, this has been diagnosed with Kanavel's signs. However, like many of these classic exams, they are not always fully present in patients.
The POCUS technique has been described beforein literature but a recently published paper did a prospective study of 57 cases. Jardin et al in Hand Surgery and Rehabilitation was at a single emergency hand care center in France. They studied patients that had any of the following: finger pain with signs of inflammation to suggest flexor tenosynovitis, confirmed infection entry portal, or pain over the flexor tendon sheath. Only those with a confirmed diagnosis were excluded.
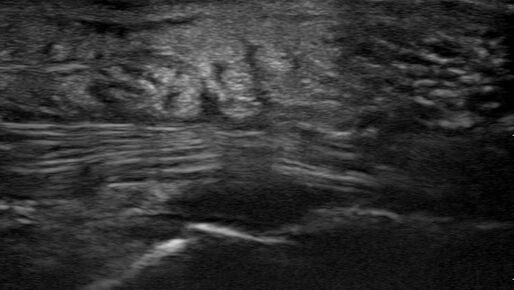
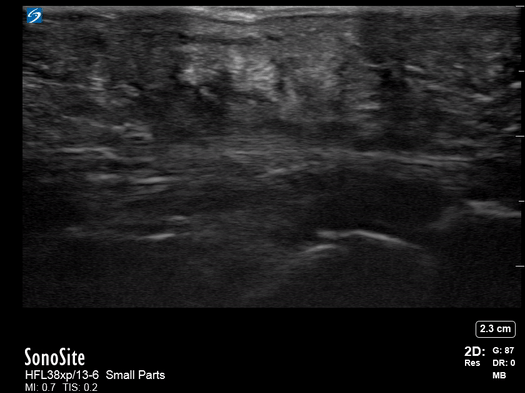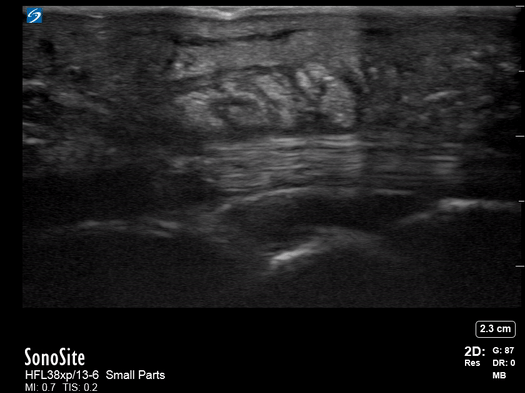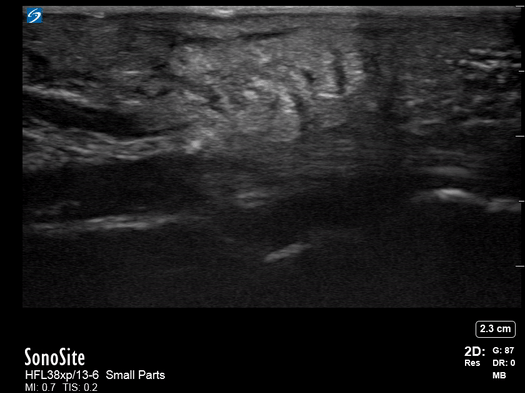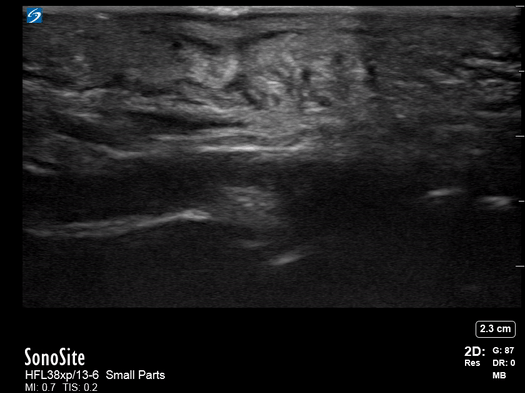
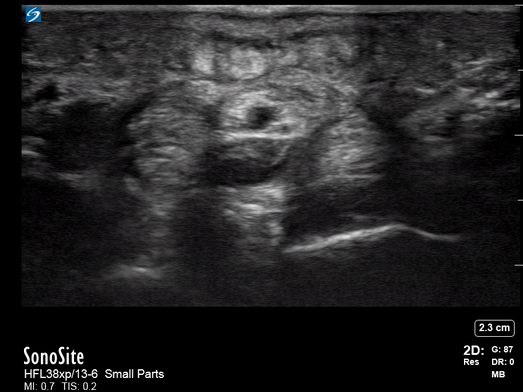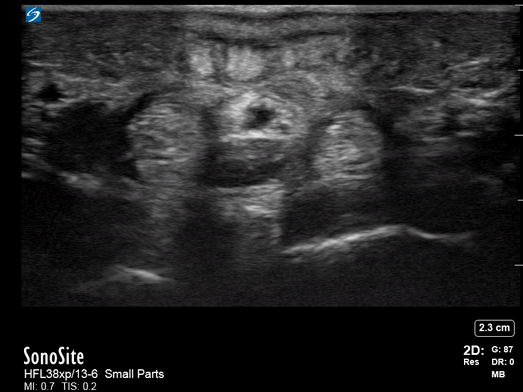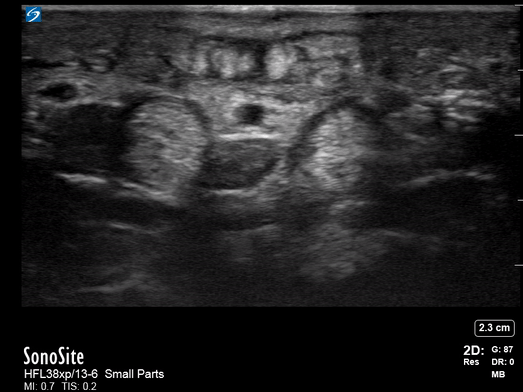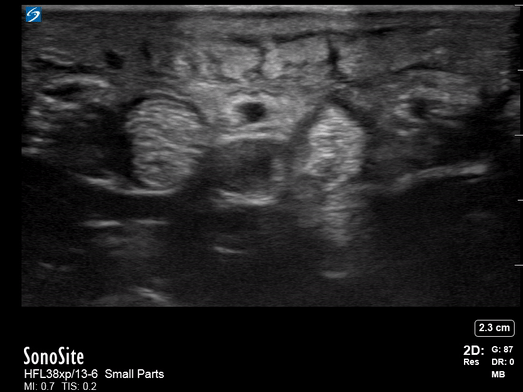
All patients were examined by a surgery resident and attending, had C-reactive protein levels draw, and x-rays performed. If the exam did not confirm the diagnosis, an ultrasound was performed. In the cases where ultrasound was positive, the patient was taken to the operating room, cultures were obtained, and pyogenic flexor tenosynovitis was ruled out if no findings were made during surgery and culture was negative. If the ultrasound was negative, the patients were treated for cellulitis with antibiotics and immobilization with close evaluation every two days until the infection improved. These patients could be taken to surgery. The individuals performing these exams were residents with at least two years of musculoskeletal ultrasound training or a senior radiologist or attending who received additional ultrasound training. They were looking for hypoechoic effusion around the tendon without signal on color Doppler, hypoechoic and hyperemic thickened synovial sheath, and the dorsal synovial recesses were examined to find effusion (suggestive of arthritis) or loose foreign bodies (suggestive of crystal arthropathy). An asymptomatic finger on the same side or the same digit on the other hand were compared as a baseline.
Of the 57 patients examined, 27 (47.4%) had peri-tendinous effusion and 23 (40.4%) had synovial sheath thickening and hyperemia. 18 of the 27 that went to the operating room were confirmed by findings or culture to have pyogenic flexor tenosynovitis. There were 10 false positive exams and one false negative that eventually went to surgery due to poor clinical outcome.
It is uncertain if these were consecutively enrolled patients, but most likely in was a convenience sample. With an overall sensitivity of 94.4% and a specificity of 74.4%. The positive predictive value was 63% and the negative predictive value was 96.7%. This study demonstrates that ultrasound is sensitive but not as specific as desired. However, there is not a discussion on whether one of the two types of findings was more accurate or how it compares to routine evaluation and management. Since the obvious cases were already excluded, it would seem to indicate that POCUS still plays an important role. There is previous evidence that with inflammatory (not necessarily infectious) flexor tenosynovitis that ultrasound is more accurate than physical exam. Let us know what you think by giving us feedback here in the comments section or contacting us on Twitter or Facebook. Remember to look us up on Libsyn and on iTunes. If you have any questions you can also comment below, email at [email protected], or send a message from the page. We hope to talk to everyone again soon. Until then, continue to provide total care everywhere.
0 Comments
Leave a Reply. |
Libsyn and iTunesWe are now on Libsyn and iTunes for your listening pleasure! Archives
August 2022
Categories |
||||||

 RSS Feed
RSS Feed