|
In resuscitation situations, such as trauma and sepsis, it is important to appropriately replace the patient's lost volume and be able to give medications in a quick and successful manner. However, what is the best way to accomplish this and why?
A common misunderstanding is that the bigger the gauge catheter, the better it is automatically. Another common misconception is that the more difficult catheters are often the "better" ones. However, a patent catheter that allows for the greatest flow is vital. However, how can we identify what is the best flow rate?
To avoid overwhelming math, let's focus on some basic principles. Flow rate is affected by viscosity of the fluid (n), pressure gradient of the tubing (P), the length of the catheter (l), and the diameter of the catheter or its radius (r). This is known as Poiseuille's Law.
In order to achieve the maximum flow, the largest diameter catheter with the shortest length should be used. Combine that with a fluid that is of low viscosity and under the maximum pressure possible. This results in the best possible flow.
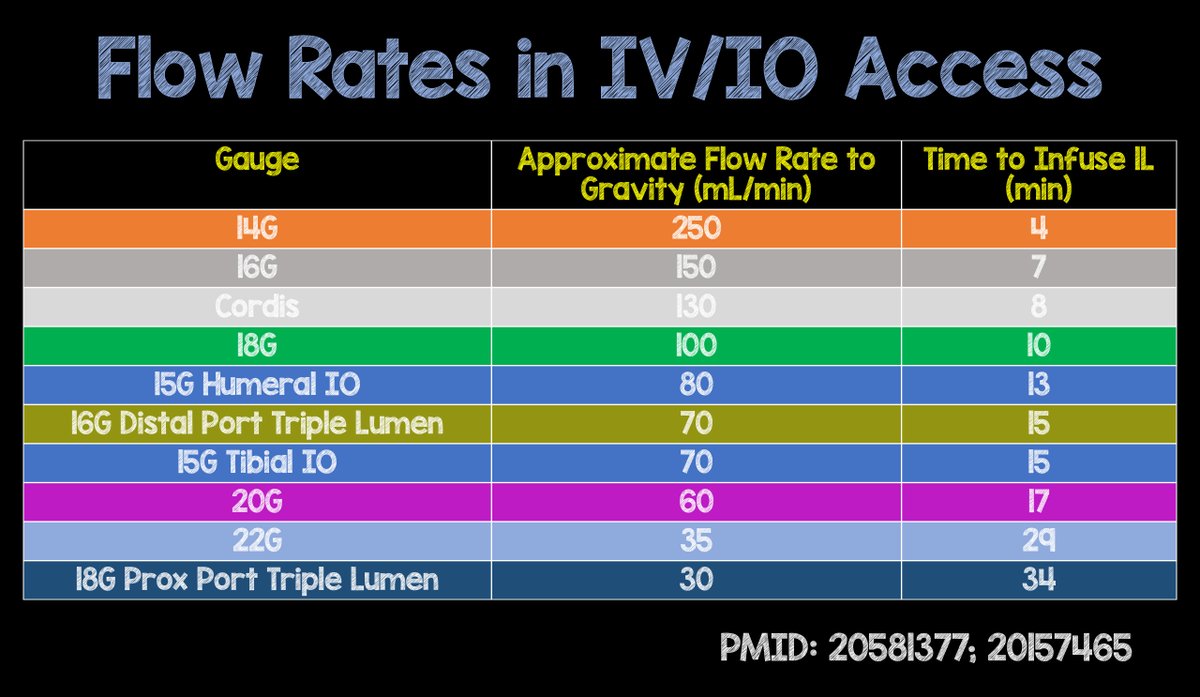
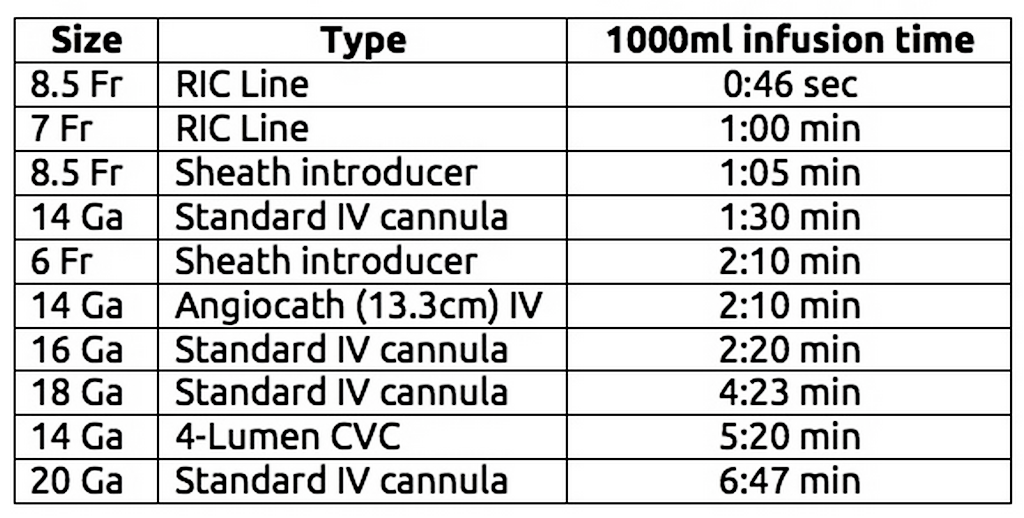
The fluid viscosity we often have little control (either the person needs crystalloids or blood products) and pressure often quickly meets a maximum. However, it does help explain why blood products take longer to infuse than crystalloid fluids and why we should use pressure bags or other devices to promote the most rapid flow possible. The biggest variables then that we have control over are the diameter and length of the catheter to achieve that maximum flow. Note the two graphs below and their varying infusion rates. One is based on flow by gravity and the other with pressure (under 300 mmHg). Also, there are some differences in the catheters listed. They both demonstrate well though the importance of picking the appropriate catheter and how much of a difference they can make.
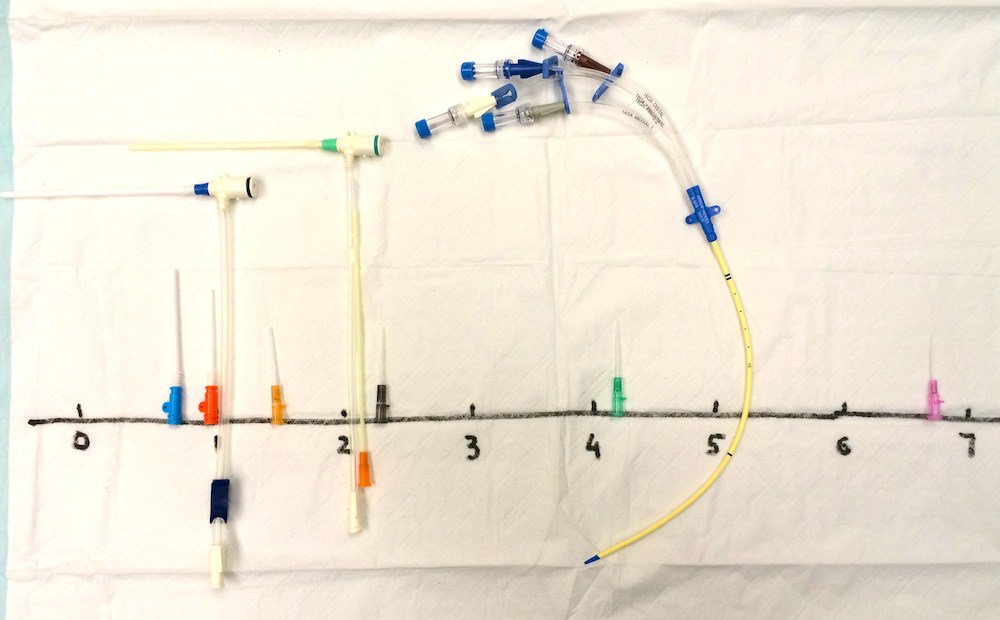
You may have also seen the picture before in social media (apologies for not being able to give credit where it is due as this has been replicated enough times that the original author is lost). What can be quickly seen is a difference not only in length but also in diameter just as was being discussed. The ones to the left are the fastest while to the right are slowest. The numbers represent the number of minutes it takes for the infusion of one liter of saline.
Despite what may often seem like the obvious choice, a central catheter may very well not be the best bet in many situations. While many departments may not have access to a Rapid Infusion Catheter (RIC), we often have access to central lines. However, a well placed 14 gauge standard peripheral line can be almost as good and a lot less hassle. While not every patient has the veins to achieve such great access, placing a triple lumen central line will most likely be counterproductive during volume resuscitation given its much slow rates compared to other types of lines.
Ultimately, the goal should be to place the catheter with the best flow rate possible for our patients during volume resuscitation. This may sometimes mean a RIC line or an intraosseous (IO) device but it is more common that a simple peripheral line will accomplish our goal well. These are also more rapid to place than the central lines that may otherwise be used. Let us know what you think by giving us feedback here in the comments section or contacting us on Twitter or Facebook. Remember to look us up on Libsyn and on Apple Podcasts. If you have any questions you can also comment below, email at [email protected], or send a message from the page. We hope to talk to everyone again soon. Until then, continue to provide total care everywhere.
0 Comments
Leave a Reply. |
Libsyn and iTunesWe are now on Libsyn and iTunes for your listening pleasure! Archives
August 2022
Categories |
||||||

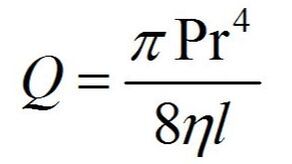

 RSS Feed
RSS Feed