|
There are a variety of anorectal emergencies that present to the emergency department. Recently, there were updated guidelines made by the World Society of Emergency Surgery (WSES) and the American Association for the Surgery of Trauma (AAST). In this post, we review some of the updated guidelines including for anorectal abscess, perineal necrotizing fasciitis (Fournier's gangrene), bleeding anorectal varices, complicated rectal prolapse (irreducible or strangulated), and retained anorectal foreign bodies.
1 Comment
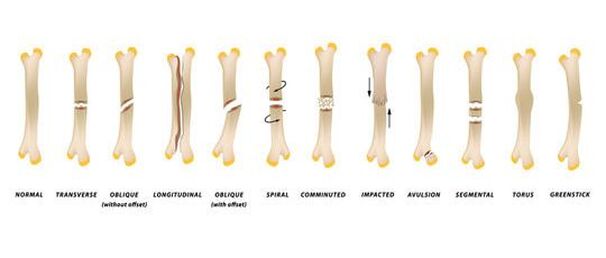
We are back to providing our ATLS content and we are picking up where we left off. Our last ATLS podcast was on spine and spinal cord trauma. Somewhat similar in nature is musculoskeletal trauma. This is a very common form of trauma. However, delayed recognition and treatment can result in life-threatening hemorrhage or limb loss.
Cluster headaches are often considered one of the most painful human experiences. They are short (lasting usually 15-180 minutes), frequent (up to 8 a day), unilateral headaches behind or around the eye often with ipsilateral autonomic symptoms and restlessness. While migraines and tension headaches are seen frequently in the emergency department, cluster headaches are much less frequently seen and often are harder to identify as a result. There are certain points to remember with patients that are experiencing cluster headaches and we list 10 of them here.
The use of tranexamic acid (TXA) has expanded with growing evidence in its use for a variety of clinical situations. However, not all evidence is created equal and not all applications show benefit. In this blog and podcast we discuss the various uses of TXA and the surrounding evidence.
For decades, there has been a major name debate regarding the appropriate title for PAs. However, on May 24, 2021 the American Academy of PAs (AAPA) House of Delegates (HOD) came to a vote. Over 100 possible titles were considered, but ultimately the winning vote was for "physician associate" which has led to a significant amount of discussion. What is the history behind this decision and why now? What has been the response? We discuss this and more in this new blog and podcast.
There are countless guides and references that can be used in emergency medicine. However, some books prove to be better resources than others and it is vital to identify them. In this post, we review one of the books you should seriously consider having if you work in emergency medicine.
Last year, the American Heart Association (AHA) provided updates to their basic life support (BLS), advanced cardiac life support (ACLS), and pediatric advanced life support (PALS) programs. Mike Sharma is helping again by reviewing some of the key updates and changes to guidelines. We also provide some additional feedback and information to consider with these new guidelines.
March is Women's History Month and we wanted to celebrate some of the accomplishments of women in medicine. While there are countless women that could be mentioned, we wanted to focus on a few that have been seen as pioneers in medicine.
Recently there was commentary in a forum that suggested the Pulmonary Embolism Rule-Out Criteria (PERC Rule) was essentially useless for detecting a pulmonary embolism (PE). It started with an anecdote, which is a logical fallacy (post hoc ergo propter hoc) and went wild from there. This led to the realization that many still do not understand how to use the Wells' Criteria for Pulmonary Embolism (referred to from here simply as the Wells' Criteria) and the PERC Rule.
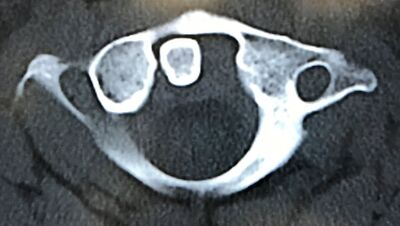
Injuries to the spine can occur both in blunt and penetrating trauma. They can also be with or without neurological deficits. For this reason, they should be considered in all patients with multiple injuries. In this podcast, Chip Lange and Mike Sharma review the pearls and pitfalls of this disease process.
|
Libsyn and iTunesWe are now on Libsyn and iTunes for your listening pleasure! Archives
August 2022
Categories |









 RSS Feed
RSS Feed